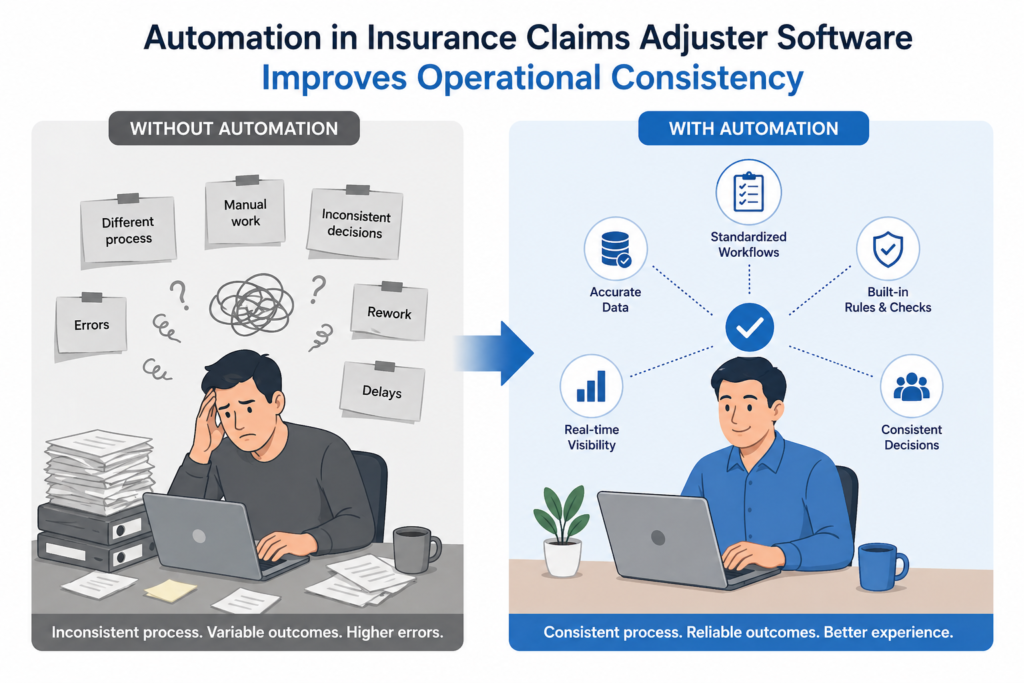
Why do policyholders complain about unfair claim treatment when insurers try to be fair? Because manual processes create inconsistency that feels unfair. Automation in claims adjuster software eliminates this perception by handling similar claims identically, building trust through consistent experiences that policyholders recognize and appreciate greatly.
Data from 2025 reveals that automated claims systems improve customer satisfaction scores by 35% through consistent handling. In response to this improvement, it’s crucial to explore key features of automated claims adjuster software, examine how automation improves operational consistency, and discuss what insurers should look for in automated insurance adjuster software.
What Are the Key Features of Automated Claims Adjuster Software?
Automated claims adjuster software offers features designed for insurance operations. Explore the key capabilities that make claims adjuster software effective.
| Software Feature | What It Does | Claims Processing Benefit |
| Data Extraction | Uses OCR/NLP on documents for key information | Eliminates errors
Accelerates validation |
| Fraud Detection | Analyzes patterns for suspicious activity | Early flagging Protects revenue streams |
| Dynamic Routing | Assigns claims by complexity and expertise | Optimized adjuster workload
Faster handling |
| Real-Time Analytics | Tracks cycle times and performance metrics | Data-driven improvements Bottleneck removal |
| Policy Integration | Syncs with core systems for coverage check | Seamless eligibility
Compliance assurance |
How Does Automation in Insurance Claims Adjuster Software Improve Operational Consistency?
Automation in claims adjuster software creates consistency across all operations. Discover the key improvements that make insurance operations more consistent.
1. Standardized Damage Assessment Protocols
Insurance claims adjusting software applies identical evaluation criteria to every claim, regardless of which adjuster handles it. This eliminates situations where one adjuster approves $3,000 while another approves $5,000 for identical damage.
- Applies uniform damage severity ratings
- Calculates labor hours using the same formulas
- References identical parts pricing across adjusters
- Eliminates subjective judgment variations between people
2. Automated Document Collection Workflows
Claims adjusting software sends the same required document requests to every claimant automatically based on claim type without human memory errors. Consistency in information gathering ensures adjusters make decisions based on complete, standardized documentation packages every time.
- Sends identical document checklists per type
- Requests missing items automatically until received
- Tracks document submission status in real-time
- Reminds claimants of pending requirements regularly
- Prevents claims processing with incomplete information
3. Uniform Fraud Detection Screening
Automated claims adjuster software runs identical fraud checks on every submitted claim to analyze suspicious patterns that humans might miss. Automated screening eliminates situations where one adjuster catches fraud while another misses identical red flags.
- Checks every claim against fraud databases
- Identifies duplicate claim submissions across systems
- Flags inconsistencies in accident descriptions automatically
- Compares damage photos with claimed repairs
- Scores fraud risk using consistent algorithms
4. Automated Approval Workflow Enforcement
Claims requiring supervisor approval automatically route upward when hitting predetermined thresholds without adjuster discretion. Every high-value claim gets management review without exceptions or forgotten escalations. Consistent approval processes prevent junior adjusters from approving claims beyond their authority limits.
- Requires manager approval above dollar thresholds
- Escalates total loss claims automatically
- Routes liability disputes to legal review
- Enforces dual approval for policy exceptions
- Tracks approval delays for accountability monitoring
5. Standardized Audit Trail Creation
Every action in automated claims systems gets logged with timestamps, user identifiers, and reasons, creating identical documentation trails. Auditors reviewing different claims see the same detail level regardless of which adjuster handled them. Consistent audit trails support compliance reviews, legal proceedings, and quality assurance evaluations effectively.
- Records every claim action with timestamps
- Documents decision rationale in standard formats
- Logs all communication attempts and responses
- Tracks document uploads and reviews chronologically
- Maintains complete claim history for investigations
What Should Insurers Look for in Automated Insurance Adjuster Software?
Insurers need to evaluate specific factors when selecting automated adjuster software. Explore the key selection criteria that guide smart selection.
I. Built‑In Fraud Warning Signs
Automated insurance adjuster software should watch for unusual claim patterns. It must flag repeated claims, mismatched damage photos, or sudden high-value requests. These alerts help insurers review risky claims early. This reduces fraud losses without slowing down honest claims.
The system should show why a claim is flagged, using simple reasons. Adjusters can then decide if deeper checks are needed. Clear fraud alerts protect insurer revenue and keep premiums fair for honest customers.
II. Fast and Clear Settlement Suggestions
The software should suggest settlement amounts based on damage, labor costs, and policy limits. This helps adjusters work faster without guessing values. Suggestions should be adjustable, so human judgment always stays in control. Speed with accuracy improves customer satisfaction greatly.
It should also show how the amount was calculated. Clear breakdowns build trust during internal reviews or customer questions. When insurers can explain payouts simply, disputes reduce significantly. Transparent settlement logic helps close claims quickly while staying fair and compliant.
III. Full Claim History and Audit Records
Reliable adjuster software must keep full claim histories. Every edit, note, photo, and payout change should be saved. This helps during audits, legal reviews, or customer complaints. Insurers stay safe when they can track decisions clearly over time.
The system should show who made changes and when. This supports accountability inside the company. Clear records help train new adjusters and improve future claim handling. A strong history log protects insurers during reviews and helps maintain clean claim processes.
IV. Simple Reports for Managers and Teams
The adjuster software should create easy reports on claim speed, costs, and outcomes. Managers need these reports to spot delays or rising losses. Clear data helps insurers improve processes without digging into raw claim files daily.
Reports should be easy to read and export. They must focus on claim trends, adjuster workload, and settlement accuracy. When teams understand performance clearly, they can fix issues early. Simple reporting supports better planning and stronger claim operations overall.
Summing Up
Insurers using automated claims adjuster software deliver consistent experiences while competitors using manual processes face mounting challenges. As claim volumes grow and complexity increases, automated insurance claims adjusting software becomes essential rather than optional for maintaining operational consistency that customers expect, and regulators demand.